Hi! How have you been? Well, I hope. I have a lot of thoughts on vaccines and variants that I want to share this week. So I will get right to it. :)
Here are a few questions that a lot of people have been asking.
How do I actually know how much immunity I have after I’ve been vaccinated with a COVID vaccine? How do I know how long immunity lasts for? Can I test for it?
Fear not, dear reader, for I have addressed these questions in my new column in Hindustan Times this week. You can read it here.
Some of the key observations:
High levels of anti-Spike neutralizing antibodies are probably a suitable immune correlate of protection.
But that does not mean that you should go out and get antibody tests immediately if you’ve been vaccinated. For one, you’ve just been vaccinated. Your antibody levels should be high. For another, there is a great deal of variability among neutralization assays limiting their immediate clinical use. Tests are not specific or sensitive enough, and do not necessarily differentiate between different kinds of antibody epitopes on the spike. For this reason (and because the efficacy of COVID vaccines available in the US was high) the U.S. F.D.A. current does not recommend getting an antibody test after vaccination.
As I write in my piece:
Antibodies are only one arm of the immune system and there are redundancies in immunity: T cells have substantial contribution in protection against Covid-19. They can step in to offer protection when antibody levels decline or variants emerge that evade antibody recognition.
It helps to think of immune protection as a sliding scale from ideal scenario of preventing infection altogether, to asymptomatic infection, to symptomatic Covid-19 progressing in the order of mild, moderate, and severe disease requiring hospitalisation. Complete protection would result in no infection or symptoms. Incomplete protection would reduce the severity of disease.
Strong levels of neutralising antibodies that bind well to virus help prevent infection and replication in the body. However, a combination of antibody and T cells can prevent severe Covid-19 and hospitalisation. Loss of antibodies or the inability to make them might not reduce protection against serious disease. Even after infection, antibody levels wane after an acute immune response phase. However, memory B cells and long-lived plasma cells can help the immune system kickstart a rapid response on re-exposure to the virus.
With these caveats in place, it is reasonable to expect that tests will be normalized in the coming months. There are also two important conclusions we can make regarding neutralizing antibodies:
We now have a reasonable measure of how well vaccines will do in efficacy trials. UK regulators have signaled they will use neutralizing antibodies to give emergency approval to a candidate COVID vaccine instead of needing full-fledged field trials.
Scientists predicted Covaxin’s efficacy by plotting neutralizing antibodies against the efficacy of already-approved vaccines. They came up with 80% efficacy. It was remarkably close to the 78% in phase III clinical trials.
How well do vaccines work against the Delta variant?
This is a great segue into a research article just published in Nature that demonstrates that the Delta variant of SARS-CoV-2 has reduced sensitivity to antibody neutralization.
This is consistent with every single study to date showing lower real-world effectiveness against Delta after one dose for every tested two-dose vaccine. The Nature paper shows that fewer than 20% of antibodies generated after vaccination neutralize the Delta variant. You need a high level of neutralizing antibodies because a lot fewer bind to the Delta spike (compared to D614G and Alpha). You get that from two doses.
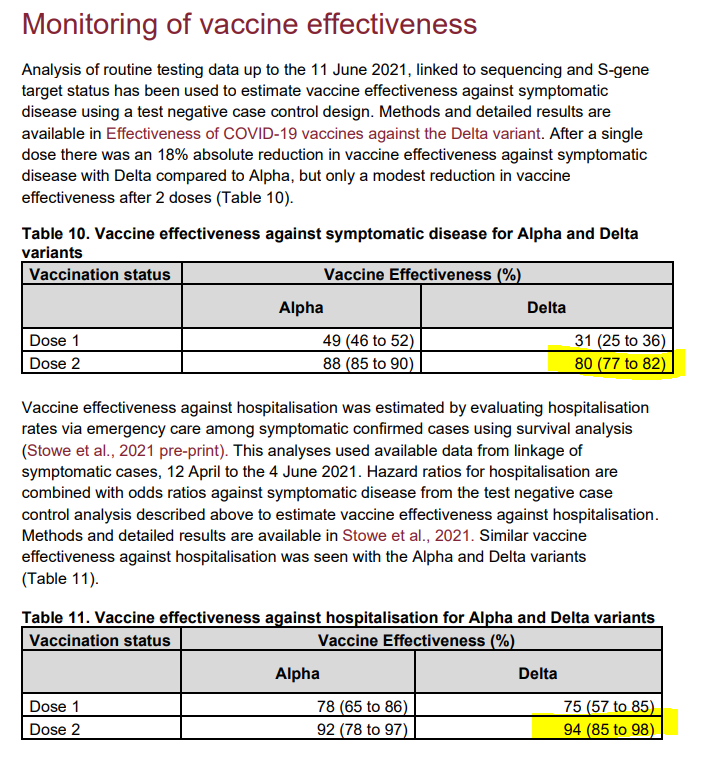
The Nature data is also consistent with the first report from Public Health England demonstrating the need for two doses of the AstraZeneca or Pfizer vaccines. I’ve highlighted the key number below.
Now, from a public health perspective, the government may prioritize giving out as many single doses to a larger swathe of the population to prevent hospitalization and death. But from a personal perspective, the numbers are clear. If you have received only one dose then you need to be very careful. I would personally not change my behaviour at all until two weeks after a second dose.
How well do vaccines work against the Lambda variant?
On June 14, the World Health Organization designated a variant C.37 first identified in Peru in August 2020 as a “variant of interest” and named it lambda. Lambda has been detected in 29 countries with a high degree of spread in Latin America. It has been detected in around 81% of cases that underwent sequencing in Peru.
Some of the first virological parameters of the variant have started to emerge from Chile in a preprint posted on medRxiv on July 1. The researchers did what is called a pseudotyped neutralization assay in which a harmless virus is covered with the spike of the variant of interest and tested for neutralization with plasma samples that contain antibodies.
Plasma samples were obtained from healthcare workers who were fully vaccinated with two doses of The Sinovac-CoronaVac inactivated vaccine.
What is the mutational profile of Lambda? The authors note the following:
The spike protein of the Lambda variant has a unique pattern of 7 mutations (Δ246-252, G75V, T76I, L452Q, F490S, D614G, T859N) of which L452Q is similar to the L452R mutation reported in the Delta and Epsilon variants . The L452R mutation has been shown to confer immune escape to monoclonal antibodies (mAbs) as well as convalescent plasma.
The authors then determine from their assays that the Lambda spike protein confers greater fitness (infectivity) than D614G (the virus prevalent in most of 2020) and the Alpha (first identified in the UK) and Gamma variants (first found in Brazil)
Neutralization was about three times less for the Lambda variant compared to D614G and roughly two times less than for Alpha and Gamma. Therefore some immune escape due to mutations can be inferred.
The key questions for me are how does this variant compare to other variants like Beta (first identified in South Africa) and Delta (first identified in India)? And how do other vaccines fare in neutralizing the variant?
These questions were not addressed directly since the authors did not compare these variants, nor did they test other vaccines. As I mentioned in the section above, comparing data from different neutralization assays is a bit risky. However based based on the numbers provided in this one preprint it looks as if the reduction in neutralization is less with Lambda than it is with Beta or Delta (there is less immune escape). As such, we can maintain cautious optimism at this time that vaccines that are more effective than CoronaVac might fare reasonably well in neutralizing Lambda. Each vaccine will have to be tested separately and we will require more data, so this optimism could be misplaced. Also, there are different epitopes and mutations can change critical ones based on the specific vaccine. But right now based on the limited data available, this is a reasonable guess.
Nonetheless, we should also remember that CoronaVac is not the most effective vaccine. Recent real-world studies in Chile have shown that CoronaVac is only 66% effective versus 93% for the Pfizer vaccine.
Does it matter what time of day you get your COVID-19 vaccine?
Given the high efficacy of COVID-19 vaccines against diverse populations vaccinated at different times of the day, the answer is “probably not”.
But it isn’t a random question either. Here's a study from a few years ago that found flu shots in the morning elicited more neutralising antibodies than those taken in the afternoon.
Given that sleep enhances immunity and that immune systems follow the circadian rhythm like every other part of the body, it is worth following up on in due course.
What else I’ve read:
Researchers at MIT and Harvard have developed wearable facemask prototype that also tests for SARS-CoV-2. It doesn’t require a swab stuck up in your nose and the results are available in 90 minutes. It is also reasonably sensitive and specific.
How COVID-19 causes brain fog.
Here is a great long article on the gut microbiome.
Nature has a sobering story that the poorest countries will not receive COVID-19 vaccines until 2023.
Here’s a thought-provoking book that starts from two irrefutable facts:
Humans are not biologically suited for space-travel.
All life on Earth will become extinct.
Starting from these two facts, the author builds a book on the idea that humans have an obligation to travel into space to preserve life, and the only way we can sustain this is through genomic engineering ourselves for space-travel.
The central thesis is humans have a duty to preserve life through space-travel which is possible only by genetically engineering ourselves.
Some salamanders can regenerate body parts. How do they do it? And can humans one day do it too?
Why is it so difficult to be happy?
This talk by Harvard’s Daniel Gilbert at the Royal Society is superlative.
Spotted in the wild ;)
Vishal spotted and shared a photo of COVID-19: Separating Fact from Fiction at a bookstore in Noida. It’s always good to see a photo of a book in the wild. Which reminds me to tell you that my book will be available on Amazon in the US from August 1. It is already available to preorder in the US. Thanks to everyone who has read, shared, and commented (even the lone person out of 50 raters who gave it a two-star on Amazon). :))








Thank you Sir for taking efforts and sharing your scientific insights in a simple language for us. 🙏